Revolutionary Compassion: Preventing Blindness in War-torn Countries
A Conversation with Adrian Hopkins, MD
Director, Mectizan Donation Program, Task Force for Global Health
Julie: Adrian, thank you so much for your willingness to share your story with The Center for Compassion & Global Health. Let’s begin with your initial work as a missionary in the Congo. How did this opportunity come about?
 Adrian: It all began when I was a medical student in Scotland. At St. Andrews University we were offered the opportunity to participate in electives, what you call “internships” in the US. I had three months where I was allowed to do anything provided it was medical. As a Christian, I felt that I didn’t want to study medicine for medicine’s sake or for the earning potential. I wanted to apply whatever training and skills I developed to help people in deep need. As I considered which elective I might take, I met a missionary doctor who was on leave from Congo and he said, “Why don’t you come and join us for three months?” His invitation appealed to my spirit of adventure so I agreed. It was September of 1969. I remember this because shortly afterward I was in the Congo listening to the report of the astronauts landing on the moon through a crackling shortwave radio.
Adrian: It all began when I was a medical student in Scotland. At St. Andrews University we were offered the opportunity to participate in electives, what you call “internships” in the US. I had three months where I was allowed to do anything provided it was medical. As a Christian, I felt that I didn’t want to study medicine for medicine’s sake or for the earning potential. I wanted to apply whatever training and skills I developed to help people in deep need. As I considered which elective I might take, I met a missionary doctor who was on leave from Congo and he said, “Why don’t you come and join us for three months?” His invitation appealed to my spirit of adventure so I agreed. It was September of 1969. I remember this because shortly afterward I was in the Congo listening to the report of the astronauts landing on the moon through a crackling shortwave radio.
After finishing a couple of years of medical residency, I was invited back to work in a remote, forested area of the Congo. The bush hospital where I practiced medicine was very isolated. Some of my colleagues found it claustrophobic due to our being surrounded by the forest. The area was described as a green box with a blue lid because everywhere you looked you saw only green forest and the sky. In those days, the hospital served 150,000 people from a landmass the size of Rwanda. Obviously, not everyone could come to the hospital because some lived too far away. We tried to deliver health services to remote areas but it was not easy. The roads were challenging; many were impassable. Also, this was the time of Mobutu’s reign and the economy was struggling. We treated anyone whether they were able to pay for services or not. When the state provided no funds, we received external support from organizations and were able to keep functioning on an even keel.
 In the early 1980’s we set up what would now be called a “community-directed program” for vaccinations. I secured funding for a few kerosene refrigerators that were strategically placed throughout the area. Local health center nurses ran the program. The villages would choose someone to come and collect the vaccines and bring them back to the communities, sometimes cycling up to forty kilometers. This typically occurred during the night so that the vaccines could arrive first thing in the morning. We were able to achieve higher coverage than with our mobile team, and this program was much, much cheaper to run. We learned the importance of decentralization. I was in this location for most of seventeen years. During this time, I also finished my residency in ophthalmology because of my interest in treating blindness, particularly cataract blindness, which accounts for nearly 50% of all blindness in most poor communities.
In the early 1980’s we set up what would now be called a “community-directed program” for vaccinations. I secured funding for a few kerosene refrigerators that were strategically placed throughout the area. Local health center nurses ran the program. The villages would choose someone to come and collect the vaccines and bring them back to the communities, sometimes cycling up to forty kilometers. This typically occurred during the night so that the vaccines could arrive first thing in the morning. We were able to achieve higher coverage than with our mobile team, and this program was much, much cheaper to run. We learned the importance of decentralization. I was in this location for most of seventeen years. During this time, I also finished my residency in ophthalmology because of my interest in treating blindness, particularly cataract blindness, which accounts for nearly 50% of all blindness in most poor communities.
Julie: In addition to living and working in the Congo, I understand you spent six years working with the Ministry of Health developing the Mectizan distribution program in the Central African Republic during a time of conflict. What was it like to keep a public health program running in the middle of such complexity?
Adrian: The African river blindness program was split into two areas, one of which was the West African Programme. Before Mectizan was available (the drug used to treat onchocerciasis or river blindness), we had another drug we could use, diethylcarbamazine (DEC), which would kill the parasite. However, if you had ocular onchocerciasis, DEC could create dangerous inflammation in the eye leading to severe visual impairment and blindness more rapidly than the disease itself. Therefore, the West African Programme focused its efforts on controlling the vector of onchocerciasis, which is a black fly. But vector control was too expensive to expand into countries such as Nigeria, a country with a lot of river blindness, so we needed a better solution.
At this point, I was working with Christian Blind Mission (CBM). In communities where onchocerciasis was very prevalent, there were many blindness rehabilitation projects. We would try to prevent blindness from happening in the first place—such as childhood blindness caused by vitamin A deficiency, or by providing cataract surgery to elders—but when it came to river blindness we could only offer rehabilitation and social integration for people with disabilities. The eye-care NGOs (e.g. Sightsavers, CBM, Helen Keller International, International Eye Foundation) were involved in rehabilitation of the blind. But once Mectizan became available, the NGOs came together under the umbrella of the World Health Organization (WHO) Prevention of Blindness unit and began to coordinate their efforts to distribute this new, more economical, and much safer solution. This occurred in areas outside of the West African Programme, which eventually developed into the African Programme for Onchocerciasis Control.
In the Central African Republic, it was not a peaceful time, but the population really banded together. Once when I was evacuated, my staff stepped in during calm periods and worked for no salary because of their commitment to the population. They had access to Mectizan and were committed to treating river blindness. I learned that when you have a good program and it’s valued, people find a way to keep it going even in the midst of severe conflict. We even used the military at some stages to distribute the drugs because the military needed to establish positive rapport with the population.
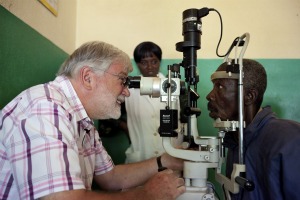 I visited Central African Republic eighteen years later for the twenty-fifth anniversary of the Mectizan Donation Program. We gave a certificate of long service to a man who had started distributing Mectizan for river blindness in 1994 and was still doing it. Some of these guys had to take leave for short periods and hide in the bush when the conflict was bad, but they came back. One man at the gathering said to me, “I came to see you in 1994 because I was going blind. You told me you couldn’t do anything for my eyes because my eyesight was gone. All you could offer was to help rehabilitate me. And, I’m still here. I recognized your voice after almost twenty years. But what’s really important is that here in this village, no one else has gone blind since you started the eye care program.” I was involved in the Mectizan effort in Central African Republic for six years and then we went back to Congo.
I visited Central African Republic eighteen years later for the twenty-fifth anniversary of the Mectizan Donation Program. We gave a certificate of long service to a man who had started distributing Mectizan for river blindness in 1994 and was still doing it. Some of these guys had to take leave for short periods and hide in the bush when the conflict was bad, but they came back. One man at the gathering said to me, “I came to see you in 1994 because I was going blind. You told me you couldn’t do anything for my eyes because my eyesight was gone. All you could offer was to help rehabilitate me. And, I’m still here. I recognized your voice after almost twenty years. But what’s really important is that here in this village, no one else has gone blind since you started the eye care program.” I was involved in the Mectizan effort in Central African Republic for six years and then we went back to Congo.
Julie: What is it that propels you to return to work in such challenging circumstances?
Adrian: One reason is that people who live in areas of conflict suffer from decisions that are made not by them, but by other people. Their healthcare suffers, among other things. During the war in eastern Congo, an average of 3,000 people died everyday. Most of the death was due to malnutrition, lack of basic healthcare, lack of hygiene, and no clean water. Nearly four million people died, and the international media ignored it because it happened far off in the middle of the Congo. How do we help the innocent sufferers? This is one reason that makes me go back.
 In Congo during the civil war, we set up an ophthalmology training center in Kinshasa, and it’s still going. People began to think, let’s not destroy our healthcare or our education or other services we need. Instead, let’s try for peace and build on that. The potential for peace building also kept me involved.
In Congo during the civil war, we set up an ophthalmology training center in Kinshasa, and it’s still going. People began to think, let’s not destroy our healthcare or our education or other services we need. Instead, let’s try for peace and build on that. The potential for peace building also kept me involved.
When I was engaged in clinical medicine, it was the patient’s recovery that kept me going. When I was practicing ophthalmology and performing cataract surgery, it was the patient regaining his or her eyesight that kept me going. Seeing some of my former students in Kinshasa who are now senior ophthalmologists keeps me going. Being able to say that there are virtually no new blind patients due to river blindness is strong motivation to continue and complete the job. We have elimination in sight.
Julie: What is the role of compassion in this front line work?
Adrian: This work stems from empathy. When you’ve been in a front line situation, you feel with the population. I started off in clinical medicine where I dealt with patients in the UK. I didn’t have long-term patients in hospital medicine. But when I lived in a community in Africa and I was their doctor, I got to know the people, some of whom became patients. You get to share in both the joys and the sorrows of the community you serve.
I remember when we had a cholera epidemic and we had no IVs. Sylvia (my wife) and I were up every night. We had to take water from the creek and filter it four times through normal gravity filters. We had some pure sodium chloride and we had bottles we could re-sterilize, but only a small number, so we were constantly producing IVs, three or four lots everyday. We worked until midnight, then got up at five a.m. and started the next lot, as well as treated the patients. When someone died, culturally it was important to hug the body, but if we allowed this then others would become contaminated. I went out into the villages and said, “Look, I know your culture, I’ve been here long enough. I know what you want to do when someone dies, but please just listen to me for the moment. When someone dies, take two or three people, bury that person, cover them up, and have your ceremonies six months down the road.” They listened, because they had confidence in me, and the epidemic finished in no time.
Julie: Is spirituality a motivating factor in your work?
 Adrian: My motivation began with an initial Christian commitment of wanting to help people, and developing the internal resources to maintain this conviction. Christian philosophy and faith supports this mindset. I had a lot of advantages growing up. Giving back was important. In the end, the question I will ask is, “Have I used my training, skills, and gifts the best that I was able?”
Adrian: My motivation began with an initial Christian commitment of wanting to help people, and developing the internal resources to maintain this conviction. Christian philosophy and faith supports this mindset. I had a lot of advantages growing up. Giving back was important. In the end, the question I will ask is, “Have I used my training, skills, and gifts the best that I was able?”
I have peace of mind and I trust in how life evolves. For example, a few years ago I would never have imagined being in my current position. I had to leave Africa due to health conditions and two days later I received a phone call from Bjorn Thylefors (then Director of the Mectizan Donation Program) who said he was retiring and would I like to take over. That timing was absolutely perfect.
Julie: Based on your experience in Africa, what message do you have for young people entering the field?
Adrian: Public health is becoming theoretical and more of an academic exercise. You study statistics, you study public health principles, you get an MPH. This worries me. Students need to be in the field at the grassroots level. This is how they will develop empathy and the inner resources to help populations, the poorest of the poor. You need to spend a year or two or three at least in an impoverished culture to understand what this means, and to gain the confidence of the population. I became a village chief in Congo after many years. I kept thinking, maybe now I understand the culture a little bit better, but there was so much more to learn. Visits to the field are fine but it’s living in those environments that will allow global health students to develop the empathy and understanding that are required to do this work.
 Adrian Hopkins, MD, has spent decades addressing blindness in African countries. During his career, he was technical advisor to the Central African Republic Ministry of Health for the National Programme for Onchocerciasis Control; established the Training Centre for Ophthalmology for Central Africa (CFOAC); has been Medical Advisor for CBM (Christoffel-Blindenmission) for the Central African Region; has served four years on the Technical Consultative Committee of APOC; and has completed four years as chairperson of the NGDO coordination group for Onchocerciasis Control. He has also been involved in national planning and implementation of the WHO Vision 2020 program to eliminate avoidable blindness, mostly in French-speaking regions of Africa.
Adrian Hopkins, MD, has spent decades addressing blindness in African countries. During his career, he was technical advisor to the Central African Republic Ministry of Health for the National Programme for Onchocerciasis Control; established the Training Centre for Ophthalmology for Central Africa (CFOAC); has been Medical Advisor for CBM (Christoffel-Blindenmission) for the Central African Region; has served four years on the Technical Consultative Committee of APOC; and has completed four years as chairperson of the NGDO coordination group for Onchocerciasis Control. He has also been involved in national planning and implementation of the WHO Vision 2020 program to eliminate avoidable blindness, mostly in French-speaking regions of Africa.