For the Common Good:
The Impact of Compassion on Global Health Programs
A conversation with Alison Krentel
Honorary Fellow, London School of Hygiene and Tropical Medicine
Julie: Alison, I am grateful that we have the opportunity today to hear about your work in mobilizing communities, working with mass drug administration (MDA) for neglected tropical diseases, and now capturing stories from the field about why, or why not, community members are willing to take medication for one of those diseases, lymphatic filariasis (LF). Let’s begin with what brought you into the field of global health.
Alison: Not art history! I studied art history as my undergraduate degree, and I love art history – 17th century Dutch painting was my area of interest, Johannes Vermeer – but I didn’t know what to do with my life as an art historian. I come from a long line of helpers in my family – teachers, doctors, nurses, and ministers – so I suppose that pull to help was a part of me as well.
 I had a strong desire to travel after I graduated and I had always wanted to go to Africa, so in 1995, I began HIV/AIDS work in Addis Ababa. At that time there wasn’t a lot you could do for people with AIDS except help them die. I worked with a church-based organization that provided minimal medical care and loans for people with HIV. We loaned people money and then forgave their loans when they died. While alive, they would hopefully start a small business that would allow their family to earn money after they died. When I returned back to Addis six months after I had left, every one of the women I worked with had died. This was an intense introduction into the world of suffering for a 22-year-old college graduate, a powerful introduction to global health.
I had a strong desire to travel after I graduated and I had always wanted to go to Africa, so in 1995, I began HIV/AIDS work in Addis Ababa. At that time there wasn’t a lot you could do for people with AIDS except help them die. I worked with a church-based organization that provided minimal medical care and loans for people with HIV. We loaned people money and then forgave their loans when they died. While alive, they would hopefully start a small business that would allow their family to earn money after they died. When I returned back to Addis six months after I had left, every one of the women I worked with had died. This was an intense introduction into the world of suffering for a 22-year-old college graduate, a powerful introduction to global health.
Julie: You mentioned your family. Is there anyone in particular who modeled compassion for you?
 Alison: My grandfather. I grew up in the States but he lived in Canada. Often when we went to visit him there was somebody staying upstairs in his home – an alcoholic drying out, or somebody with drug addiction problems. At many family gatherings and meals, someone who Grandpa was helping would join us. My grandfather was a surgeon and a General Practitioner in a rural area of Quebec and was an extraordinary man. He had a heart for helping people. He received the Order of Canada for his service to humanity in that region of Quebec, which was a great family honor.
Alison: My grandfather. I grew up in the States but he lived in Canada. Often when we went to visit him there was somebody staying upstairs in his home – an alcoholic drying out, or somebody with drug addiction problems. At many family gatherings and meals, someone who Grandpa was helping would join us. My grandfather was a surgeon and a General Practitioner in a rural area of Quebec and was an extraordinary man. He had a heart for helping people. He received the Order of Canada for his service to humanity in that region of Quebec, which was a great family honor.
Julie: As a child how did that affect you? What was it like to witness your grandfather inviting in strangers?
Alison: For our family it was normal. My dad was a minister in the church. Every Sunday we had lunch and stray people would join us. It didn’t matter who it was. My mother never knew how many people would be at our table for lunch, and it was fun. A lot of my family is like this.
Julie: How did this compassion lead you to global health and a focus on LF elimination?
Alison: I probably ended up in global health primarily because I love to travel. That is what got me out the door, so to speak. But then, in Ethiopia, I felt that I was doing something good, something to help. Those early experiences impacted me. I recognized that we are all equal. I’m not better than anybody else and they’re not better than me, and that we all have similar needs and desires. I have an obligation to serve those who don’t have the same access to basic needs, who don’t have the same opportunities as I do. It’s trying to right the wrong, trying to fix what isn’t fair, giving people a better opportunity and putting myself in their shoes in the process. You don’t do global health work for the money, and you don’t do it because it’s easy.
Julie: You’ve mobilized communities and healthcare systems for LF elimination activities. Why are some communities and organizations responsive to the invitation to engage in LF elimination activities, while others are not? What role might compassion play?
 Alison: Compassion is very important, and a lack of compassion can also have a significant impact. In 2002, in Alor district in Indonesia, we worked very closely with six communities to demonstrate that a community-directed LF treatment program could work in Indonesia. Five of these communities were very compassionate and easily mobilized their efforts to alleviate suffering. However, the sixth village was led by a village leader who was hard to work with. His attitude was abrupt; people in his village were afraid of him. We were told that he was associated with black magic. Even our Indonesian team was afraid to work there and our driver very firmly told me that we were not allowed to spend the night in this community. We found the village itself dirty, people didn’t seem to take pride in their homes or gardens and people were not emotionally open and as willing to work with us as in the other five villages. It was a very difficult place to work.
Alison: Compassion is very important, and a lack of compassion can also have a significant impact. In 2002, in Alor district in Indonesia, we worked very closely with six communities to demonstrate that a community-directed LF treatment program could work in Indonesia. Five of these communities were very compassionate and easily mobilized their efforts to alleviate suffering. However, the sixth village was led by a village leader who was hard to work with. His attitude was abrupt; people in his village were afraid of him. We were told that he was associated with black magic. Even our Indonesian team was afraid to work there and our driver very firmly told me that we were not allowed to spend the night in this community. We found the village itself dirty, people didn’t seem to take pride in their homes or gardens and people were not emotionally open and as willing to work with us as in the other five villages. It was a very difficult place to work.
Later, the transmission assessment surveys showed a little hot spot in Alor where transmission of LF continued. I asked the team who completed the survey where it was and they confirmed that it was that sixth village where we had difficulty working. It seemed that a lack of compassion filtered down from that village leader into the community and promoted a culture of fear. People could not be mobilized. Thankfully most of the villages in Alor that I worked in were not like that. Instead we found leaders who had compassion and were willing to mobilize their communities, provide water and supplies during the MDA and promote taking the pills.
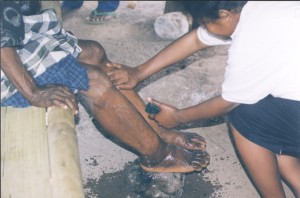 When I think about the role compassion plays in mobilizing communities, I think of the nurses and midwives who modeled compassion and care, and those that benefited directly from their compassionate acts. Again in the Alor district, we were demonstrating leg washing in one village where the LF rate was over 20%. My Indonesian language skills were not very good at the time. The woman whose leg we were washing began to cry, tears streaming down her face. I remember saying to the nurse, “Stop, you must be hurting her, we must stop the demonstration.” The nurses explained to me that, no, she was crying because nobody had touched her for years. This moved me deeply. It was something I had never expected.
When I think about the role compassion plays in mobilizing communities, I think of the nurses and midwives who modeled compassion and care, and those that benefited directly from their compassionate acts. Again in the Alor district, we were demonstrating leg washing in one village where the LF rate was over 20%. My Indonesian language skills were not very good at the time. The woman whose leg we were washing began to cry, tears streaming down her face. I remember saying to the nurse, “Stop, you must be hurting her, we must stop the demonstration.” The nurses explained to me that, no, she was crying because nobody had touched her for years. This moved me deeply. It was something I had never expected.
Other great examples of compassion include those who work until all hours of the night delivering drugs and making sure that people who took the medication aren’t having side effects. In Alor in those early days, people were afraid of side effects after the first time they took the drugs. I remember women who stayed up late into the night walking through the village with their flashlights, checking on people, delivering Paracetomol and making sure everyone was okay. The power of community is extraordinary, and if you can tap into that it’s like magic, it really is.
For me compassion is putting yourself in someone else’s shoes. I think about the people in the field who are delivering these medications year in and year out. How do they feel, and how do we make it better for them? We are putting a whole lot of pressure on them to succeed, and what are we doing to help them? I feel a lot of compassion for the people for whom we are trying to serve with the drug distribution, but I also feel a lot of compassion for the community health workers who are implementing these programs. How do we help them so they don’t get forgotten in the process?
Julie: You’ve studied the factors that are associated with high and low drug coverage of MDA for LF. Compassion is not usually studied as one of these factors, but from your experience what role does it play for drug distributors and for the populations themselves?
Alison: Compassion plays a huge role in drug distribution, particularly the compassion of those who distribute the drugs in the communities. Directly-observed treatment (in which the drug distributor observes the person taking the medicine) requires a relationship of trust. By that, I mean that if I, as a volunteer community health worker, take time to be with you, to listen to you, to explain why I am here delivering medication to you, you will be more likely to trust me and swallow the pill I’ve just handed you.
 The person who dispenses the drugs needs to have compassion for the recipient, to understand how that person is feeling, the concerns they might have, their questions and fears. What if my child gets a fever? Do I have to take him to the health center tomorrow because he is reacting to the medicine? What if I don’t have any money to pay the health center? Or understanding the complex interaction within a family… in some situations I have seen, the husband forbids the wife from taking the drug. What’s going on there? It’s beyond the realm of a drug distributor to solve these issues, but if they have compassion, if they understand the person they’re giving the drug to has needs and concerns and fears, then we will all understand better when there is resistance to taking the medication.
The person who dispenses the drugs needs to have compassion for the recipient, to understand how that person is feeling, the concerns they might have, their questions and fears. What if my child gets a fever? Do I have to take him to the health center tomorrow because he is reacting to the medicine? What if I don’t have any money to pay the health center? Or understanding the complex interaction within a family… in some situations I have seen, the husband forbids the wife from taking the drug. What’s going on there? It’s beyond the realm of a drug distributor to solve these issues, but if they have compassion, if they understand the person they’re giving the drug to has needs and concerns and fears, then we will all understand better when there is resistance to taking the medication.
There are studies that show repeat visits to the community are associated with greater acceptance of MDA. I believe that these repeat visits build relationships and foster trust making it more likely that people will take the drug. Compassion, respect, and trust are required for the volunteer distributor, the person who receives the drug, the health service staff, and the program managers for all of this to work.
 For many people, taking the LF medication could be seen as an altruistic act, because they aren’t sick or don’t have any symptoms and they report taking it for the benefit of their community. At the end of the day we are asking for a lot of altruism in this program. We are asking drug distributors to work for free or for very little, and we are asking people to take pills that might make them sick even though they’re not sick. I think altruism is a big part of LF elimination.
For many people, taking the LF medication could be seen as an altruistic act, because they aren’t sick or don’t have any symptoms and they report taking it for the benefit of their community. At the end of the day we are asking for a lot of altruism in this program. We are asking drug distributors to work for free or for very little, and we are asking people to take pills that might make them sick even though they’re not sick. I think altruism is a big part of LF elimination.
Julie: Some of your work now includes capturing stories. Why stories, and what are they revealing?
Alison: We are wrapping up two years of research in Indonesia using micro-narratives, or stories, to help us better understand the success of drug delivery programs. We asked community members in two districts about their experiences when receiving the LF drugs, and the people delivering the drugs about their experiences. In one of the districts the drug delivery program had failed, and in the other district the program was underperforming. The stories we captured helped both of these districts improve their MDAs and make significant changes towards success.
Julie: How do they apply the stories?
Alison: These are short stories, maybe five lines. The stories provide an open door to bring you into an experience, a salient experience. In traditional surveys we ask a lot of questions such as what do you know, what do you think, what do you believe. Our story survey asks, “What happened to you?” This is a more powerful question for improving a program. The recipient of the medication might know that LF is caused by a worm or transmitted by a mosquito. But maybe the drug distributor wasn’t very nice to you on the day they delivered the drug so you didn’t take it. Stories are a powerful way to understand how people experience the program. We share these stories with program leaders to initiate change. Our next step is topic modeling and creating word maps to try and understand the main themes within the stories.
Julie: Any particular findings that have really spoken to you?
Alison: Yes. There is a strong association between participating in MDA and the common good. If you believe you are taking the pill for the common good you will be more likely to take it. We found this in both the urban and rural areas. We sometimes think that people in cities are not as interested in their communities as those living in rural areas, but we found this same level of interest in urban Jakarta.
Julie: Acts for the “common good” has the ring of compassion to it, as well as social justice. How do compassion and social justice support each other, or not?
Alison: They are two sides of a coin. Social justice is a big component of global health, and compassion fuels social justice. Can you be a proponent for social justice and not have compassion? I don’t know if you can. I think they’re inseparable. Working for justice can be a slog, and if you’ve ever fought for justice, you know it can be a long haul. Compassion is the cheerleader saying, “keep going!” – reminding you there’s a greater good that you’re fighting for.
Julie: What have you found most meaningful about your work?
 Alison: Being in the field. That’s when I’m really fulfilled. I love being at home too, but when I think about work, that’s what I miss most, “seeing the faces” as Dr. Bill Foege says. Unfortunately the more you are in this business the more time you spend in meetings and the less you see of the people you actually want to help, and that’s the unfortunate part of it because I love being in communities talking to people.
Alison: Being in the field. That’s when I’m really fulfilled. I love being at home too, but when I think about work, that’s what I miss most, “seeing the faces” as Dr. Bill Foege says. Unfortunately the more you are in this business the more time you spend in meetings and the less you see of the people you actually want to help, and that’s the unfortunate part of it because I love being in communities talking to people.
Julie: What challenges have you faced?
Alison: It’s a challenge in our business that we don’t have a forum in which to champion people. I think we could inspire each other more than we do. Maybe it’s the nature of the work that we do, being spread across the globe that makes it more difficult to do this. I think it’s good to celebrate people, and not just their achievements but also their person. These inspirational interviews you are producing about compassion and global health celebrate people and I’m grateful for that. We need to champion people, and that’s what your interviews do. I’m always inspired by what I read.
 Another challenge for me is that we haven’t paid a lot of attention to the reasons why people do what they do. The questions we have can be answered by a behavioral psychologist or an anthropologist, but not always with easy, neat answers. It’s a battle to get those questions put on the agenda because we measure them differently than through a randomized control trial. People are people, and they’re crazy and messy and hard to understand and they don’t make sense and they’re irrational… and we have to keep trying to understand them and ask questions anyway. For us, knowing why people do or don’t take a drug is crucial to the success of our programs. We haven’t always taken the time to understand and find the answers to those questions.
Another challenge for me is that we haven’t paid a lot of attention to the reasons why people do what they do. The questions we have can be answered by a behavioral psychologist or an anthropologist, but not always with easy, neat answers. It’s a battle to get those questions put on the agenda because we measure them differently than through a randomized control trial. People are people, and they’re crazy and messy and hard to understand and they don’t make sense and they’re irrational… and we have to keep trying to understand them and ask questions anyway. For us, knowing why people do or don’t take a drug is crucial to the success of our programs. We haven’t always taken the time to understand and find the answers to those questions.
Julie: What is it that sustains you?
Alison: My faith predominantly, which is behind my belief that all people are equal. I remember an experience I had when I worked with Medecins Sans Frontierès (MSF, Doctors Without Borders) in West Timor in Indonesia. It was a very tense time and we were having more and more security incidents in the refugee camps where we worked. So much so that eventually we were evacuated due to the killing of three UNHCR colleagues.
 One morning though before that happened, we needed to go back into the camps to reopen our clinic after one of these security incidents. Everyone was nervous. At that time I was the field coordinator for a HIV/AIDS project that due to the situation, now included a refugee health component. I was as nervous as the twenty-year-old Indonesian nurses I was going to send into the camps that morning. I remember thinking that as their boss, I can’t send them in if I’m not going to go, because that’s not fair. So I hopped in the car and rode in with them. The car was completely quiet because we were all terrified of the situation. During the ride, I remember thinking that my life was not worth more than the pregnant woman that we were going to go see who needed her prenatal care. And in the grand scheme of things I was only as important as she was. I thought about Jesus, the truest humanitarian, treating everyone as equal.
One morning though before that happened, we needed to go back into the camps to reopen our clinic after one of these security incidents. Everyone was nervous. At that time I was the field coordinator for a HIV/AIDS project that due to the situation, now included a refugee health component. I was as nervous as the twenty-year-old Indonesian nurses I was going to send into the camps that morning. I remember thinking that as their boss, I can’t send them in if I’m not going to go, because that’s not fair. So I hopped in the car and rode in with them. The car was completely quiet because we were all terrified of the situation. During the ride, I remember thinking that my life was not worth more than the pregnant woman that we were going to go see who needed her prenatal care. And in the grand scheme of things I was only as important as she was. I thought about Jesus, the truest humanitarian, treating everyone as equal.
Julie: Do you have any messages for young people entering the field?
Alison: Find mentors and ask questions. At every stage of your career you need a mentor, you need somebody who is just a little bit further down the line than you, who you can learn from and take advice from. Also, build relationships. Every job I have accepted was due to a relationship that led to a position. In all things, relationships are key.
 Dr. Alison Krentel, MSc PhD has worked in public health for 20 years, primarily in health promotion and community engagement for the control of infectious diseases. She spent many years working in HIV/AIDS programs in Africa and Indonesia before shifting to LF elimination and NTD programs. Together with her Indonesian colleagues, she is a founding member of Yayasan Tanpa Batas, an NGO dedicated to continuing the work MSF did in West Timor after the official mission ended in 2001. Alison teaches public health at the London School of Hygiene and Tropical Medicine and at the University of Ottawa. She is a member of the WHO Collaborating Center for Knowledge Translation and Health Technology Assessment in Health Equity at the Bruyère Research Institute.
Dr. Alison Krentel, MSc PhD has worked in public health for 20 years, primarily in health promotion and community engagement for the control of infectious diseases. She spent many years working in HIV/AIDS programs in Africa and Indonesia before shifting to LF elimination and NTD programs. Together with her Indonesian colleagues, she is a founding member of Yayasan Tanpa Batas, an NGO dedicated to continuing the work MSF did in West Timor after the official mission ended in 2001. Alison teaches public health at the London School of Hygiene and Tropical Medicine and at the University of Ottawa. She is a member of the WHO Collaborating Center for Knowledge Translation and Health Technology Assessment in Health Equity at the Bruyère Research Institute.